By Howard Mango, Ph.D., Au.D
In my last blog, I shared how Audiology serves to protect and restore our hearing healthcare and wellness, and the benefit we provide patients and physicians.

Recently I had the opportunity to travel to Indianapolis to present to colleagues at the American Academy of Audiology (AAA) conference. Our team collectively chose the subject Dizziness 2017: It’s Time To Take The Stage.
Why dizziness?
I am a vestibular specialist. Our clinical team treats dizziness, vertigo and balance disorders, and comprehensively test for vestibular function. Often we see patients who have been down what I describe as ‘the long and winding road’ searching for answers, with no relief – that journey may include primary care physicians, cardiologists, neurologists, endocrinologists –among others. According to VEDA, the Vestibular Disorders Association, 56% of patients see 4+physicians before being accurately diagnosed and treated (2014).
I believe audiologists can better manage an alternative to the many medications, unremarkable testing, home Epley maneuvers and physical therapy that are ineffective for many.
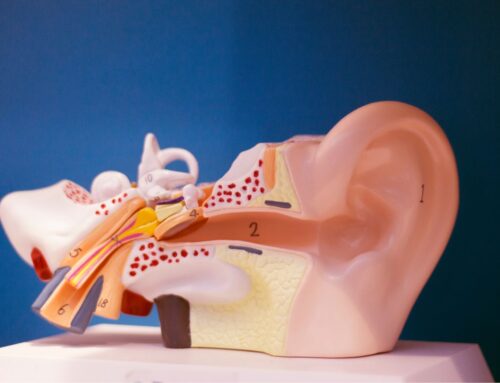
Audiologists have unique training that allows them an understanding of the anatomy and physiology of the ear as it relates to both hearing AND balance. Skillfully-trained audiologists have the resources available to evaluate, diagnose and effectively treat balance issues without referring onto outside therapies. They have the means to effectively evaluate balance dysfunction, and treat it too.
My Institute colleagues and I feel that in 2017, the time has come for the Audiology profession to better serve their balance patients with expanded, comprehensive vestibular testing and then, fully manage their patient’s vestibular rehabilitative treatment.
Testing for vestibular function involves comprehensive evaluation. This paints a picture of a patient’s overall vestibular function, not merely a small portion of it. A ‘typical balance evaluation’ may only include 2 tests. Limited testing means limited diagnosis. An independent study concluded 68% of vestibular dysfunction in patients would be missed if only one test, known as the VNG, was performed (w. Chung & Chu).
Fortunately, there are numerous tests available to assess the peripheral vestibular system comprehensively. Without these additional tests, the entire system, including the most functional parts of it, will not be evaluated. These include vestibular ocular reflex (VOR), vestibular spinal reflex (VSR) otolith function, otolith ocular reflex (OOR) as well as function of the superior and inferior portions of vestibular nerve.
Our Institute has the capability and ability using techniques and training at hand. That allows us to formulate a differential diagnosis that offers more precise information. In turn, that differential diagnosis allows audiologist to better manage, and become more directly involved, in the treatment of persons with vestibular disorders. All comprehensive testing can be completed with patient comfort in mind. Modulized testing can be scheduled to adequately accommodate each patient’s needs, including breaks to refresh and rejuvenate.
To treat balance dysfunction, traditional or conventional vestibular rehabilitation (VR) is a well-documented, exercise-based rehabilitation strategy that is customized to accommodate patients’ unique needs and goals. I believe VR demonstrates a bottom-up approach, starting with the feet and lower extremities. While it is beneficial for many individuals, it does work for everyone and for some, does not reduce symptoms or provide lasting relief. As many as half of those who undergo traditional VR demonstrate needs for rehabilitation techniques that are not fulfilled by current VR protocols. This appears to be more prevalent among those experiencing visually-induced dizziness.
So we’ve known for some time it works, but can be improved.
At times, medical management, such as imaging studies, dietary control, or referral to additional specialists is warranted. We often recommend Epley Omniax(R) treatment or Advanced Vestibular Treatment™ (AVT).
AVT is an audiologist-driven approach to the treatment of vestibular disorders.
AVT is a top-down approach to treatment, focusing on the head – inner ear, vision and communication to the brain. Goals of treatment are often to achieve further central compensation for peripheral vestibulopathy; to desensitize our patient to motion via habituation; and to reduce residual symptoms of imbalance and dizziness. It uses a pphilosophy and approach that incorporates sessions in-clinic with concurrent patient-driven home exercises. The progression of therapy is driven by subjective and objective data. AVT is fully customized for each patient.
Currently we use AVT to treat
- Peripheral Vestibulopathy
- Bilateral Peripheral Vestibulopathy
- Multifactorial Disequilibrium
- Migraine Induced Vestibulopathy
- Meniere’s Disease
- Endolymphatic/ Vestibular Hydrops
- BPPV
- Posttraumatic Vestibulopathy
- BPV of childhood
When I reflect upon the progress our Institute has documented: our staff training, expertise, protocols, Institute-led research projects and finally, the resulting positive, lasting relief outcomes by our patients, I see the potential opportunity ahead for our fellow audiologists.
Audiology has a bright future and serves an important role. Now’s the time to put the spotlight on how audiologists identify AND treat balance dysfunction. We can better serve our patients and physicians by providing more comprehensive dizziness and balance evaluations, as well as vestibular treatment, within the audiology practice.
Until next time,
Dr. Mango